Open heart surgery is teamwork performed and led by the cardiac surgeon. He is closely collaborating with the anesthesiologist and other team members throughout the procedure. In most cases, the surgery is performed on a still heart, while the heart-lung machine is replacing heart and lung function during this sensitive period. The heart spontaneously retakes acction by the of the procedure. The patient is weaned from the heart-lung machine and transferred to the ICU.
Introduction
SURGICAL APPROACHES TO THE HEART
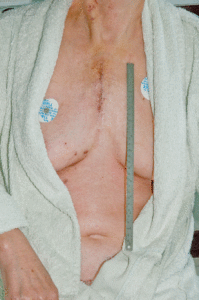
Open-heart surgery could be done through several different chest incisions depending on the procedure and general patient condition. Median sternotomy is standard and the most common access to the heart. That is a longitudinal incision through the chest bone midline that provides an excellent view for the majority of heart surgery procedures. The chest bone is closed by stainless steel wires and needs six weeks to heal after that.
Minimally invasive heart approaches reduce surgical trauma. The so-called “J” shape sternotomy is a longitutdinal cut of an upper sternum. That is frequent access for the aortic valve, but for mitral valve procedures as well. Aortic valve could be operated through a second right intercostal space equally. Superior esthetic features and less surgical trauma are justified only if a surgical team is not compromising the patient safety and the quality of a procedure. Depending on the surgery, sometimes additional small incisions could be done in groins or under the collar bone mainly for the heart-lung machine cannulation.
ENDOSCOPIC HEART SURGERY
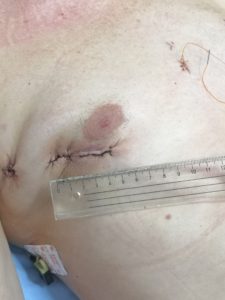
Endoscopic heart surgery is called port-access surgery. It is a video-assisted open-heart procedure performed through a small 4 – 5 cm incision through the fourth left intercostal space. Another tiny cut is necessary for the endoscopic camera. Generally, incisions are hidden and almost invisible because they are made through the nipple or in the breast fold. That is frequent access for mitral valve surgery, although tricuspid valve, some congenital heart diseases like the atrial septal defect or some heart tumors could be operated that way. The main advantage of port – access heart surgery is less surgical trauma and faster recovery. In addition to a superior esthetic effect, patients who operated endoscopically have less pain, minimal blood loss, and quicker recovery.
Port access surgery is the gold standard for the mitral valve repairs today. If performed on time and by the experienced high-volume surgical team, endoscopically repaired mitral valve patients, will be recovered and fully functional within two weeks after the surgery.
ANESTHESIA IN CARDIAC SURGERY
The anesthesiologist is taking care of painless surgery, maintains patient vitals throughout the procedure, and plays a crucial role in keeping the operation safe and stable. Altogether with a heart surgeon and an intensive care doctor, the anesthesiologist is responsible for the patient’s well being in the intensive care unit after that. Anesthesiologist intubates dormant patients before the procedure by placing a tube into the trachea. This tube is a safe airway necessary for lung ventilation during the surgery. The endotracheal tube will be removed after the surgery, providing the patient is quite awake and capable of breathing spontaneously.

HEART LUNG MACHINE

Open heart surgery is mainly done on a still heart. A heart-lung machine is installed at the beginning of the procedure to provide blood oxygenation and organ perfusion during this period. The machine roller pump replaces heart-pumping action, while the blood is oxygenated, passing through specially designed artificial lungs connected with the machine tubing system. The perfusionist is medical stuff trained to run and operate the heart-lung machine. In some cases, like coronary bypass surgery, it is possible to do a procedure without stopping the heart. That is what we call the beating heart surgery.